Not another sleepless night!
It’s time for a sleep study.
By Paula Franken
If sleep issues are affecting your life, your doctor may order a sleep study — which you might be able to do at home in the comfort of your own bed.

The at-home sleep study
You can pick up a testing kit at the sleep lab or have it delivered to your home. The kit will include:
- A breathing monitor
- A fingertip oxygen sensor
- Nasal tubing
- Instructions and contact information for the sleep lab
If more information is needed, your doctor may have you check in for a night at the sleep lab.
The in-lab sleep study
Sleep tests in the lab are available 24 hours a day. You’ll arrive one to two hours before your regular sleep time and stay through your normal sleep cycle.
Preparing for the sleep lab is easy — just stick to your regular routine. No napping, though. And avoid drinking alcohol or anything caffeinated.
Right before leaving for the sleep lab, take a shower or bath. Lotion and hair products can interfere with sensors, so don’t bother with them. Once you’re clean and ready to go, grab your overnight bag. Be sure to bring pajamas, toiletries and clean clothes to go home in.
Sleep labs at Geisinger are private rooms that feel like hotel rooms — some are even designed just for kids. Once you’re checked in, a technician attaches small sensors to your body to measure:
- Heart rate
- Oxygen saturation levels
- Sleeping position
- Eye and limb movement
- Breathing patterns
- Snoring and other sounds
After the sensors are in place, you’ll be free to read or watch television until you fall asleep. If you need anything, you’ll be able to communicate with the sleep medicine staff at any time.
What can a sleep study diagnose?
Your doctor may order a sleep study if they suspect you have any of the following sleep disorders:
- Sleep apnea
- Restless leg syndrome
- Narcolepsy
- Nocturnal seizures
- Sleep-wake cycle disorder
- Excessive daytime sleepiness
- Insomnia
Back home and sleeping soundly
After your sleep study, you and your doctor will go over the results and work on a plan to put an end to sleepless nights. Just like you’ve always dreamed.
We’re pulling back the covers on our sleep lab.
Did you know Geisinger has a sleep lab, where you’re diagnosed while you doze? It’s probably the most relaxing medical exam you’ll ever have.
Well, maybe.
One of our PA Health staffers spent the night in one and tells you what to pack — and what to expect.
My night in the sleep lab
By Jessica Martin
The thing about genetics? You don’t get to pick what family traits you get. My snoring comes courtesy of my dad’s side. He does it. His brother did it — on a camping trip, Uncle Bud’s snores wove a peculiar acoustic tapestry with ethereal loon calls. My brother does it. And, according to my husband, I do it, too.
Recently, I’ve started snorting or gasping and waking myself up. Often, I feel tired the next day, like I haven’t had enough rest. So, I asked my primary care doctor for a referral to sleep medicine.
A video visit with a sleep specialist led to an appointment to spend the night in the sleep lab.
The instructions were simple. No caffeine after noon. No lotion, because the sensors attach best to squeaky-clean skin. And bring pajamas with a top and bottom, not a single-piece nightgown.
No problem. Yet I worried that I’d get no sleep — and no data. But when I arrived for my 9 p.m. appointment and met friendly, upbeat “polysomnographic technologist lead” (aka “sleep tech”) Kristi Rhodes, I felt more at ease.
She led me to what looked like a hotel room: bed, desk, lamp, TV and bathroom. Yet there were differences: a video camera trained on the bed, a wardrobe filled with monitoring equipment, a two-way speaker on the wall and no lock on the door.
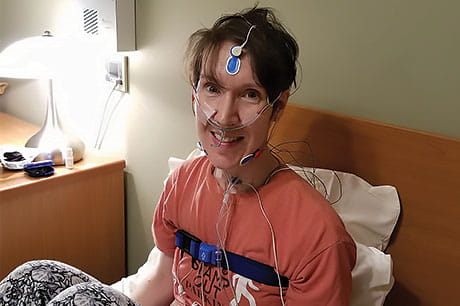
Once I was in my pajamas, Ms. Rhodes attached 20+ brightly colored wires with sticky sensor pads to my legs, chest and back, neck, jaw, face and scalp. Then a cannula for my nose and a fingertip oxygen sensor. Plus, two bands cinched around my chest and stomach. Everything was connected to a device about the size of a Kleenex box.
As she worked, Ms. Rhodes explained why different parts of my body were being monitored. Twitching leg muscles might indicate restless leg syndrome, for example. Also being checked: jaw clenching, breathing, heart rate and brain waves (to determine when I fell asleep).
Good thing I’d hit the bathroom before she hooked me up. If I had to get up at night, I’d have to address the speaker, asking for help. Ms. Rhodes would disconnect the box from the main cord, and I’d carry it, wires and all, with me.
Once Ms. Rhodes left my room, we did an equipment check. As I lay in the dark, she spoke through the speaker, giving me instructions to be sure the wires and tubes were working correctly.
“Lie still with your eyes open… Look up… Look down… Make a coughing or snoring sound… Hold your breath…”
When the tests were complete, she said good night. It was all up to me now. I breathed deeply and tried not to think about the wires. They felt weird and a bit restrictive, but not terribly uncomfortable. And after what seemed like a long time, I fell asleep.
I did wake up several times — more than I would at home. But each time, I managed to drift off again. A vivid dream involving devices with complicated wires told me I slept fairly deeply at some point.
At 5:30 a.m., a cheerful “Good morning, Jessica, time to wake up” came from the speaker and we repeated the equipment check to make sure everything had worked. Then Ms. Rhodes came in to detach everything.
Once freed, I had a chance to wash off the sticky sensor gel and answered some questions about how I felt I slept. And at 6:30 a.m., I headed home for a cup of coffee before work.
A few weeks later, I had another video visit with my sleep specialist, Katelyn Gray Smith, DO, to discuss my results. Turns out the snoring might not be the source of my fatigue after all. Those sticky sensors showed my legs move a lot — around 30 times an hour, about twice as much as average. Dr. Smith explained that even slight leg movements can wake up my brain. A lot of tiny awakenings add up to feeling less well-rested in the morning.
A quick blood test revealed low iron levels. Topping up my body’s supply with some over-the-counter iron supplements can ease the twitchiness of my leg muscles, leading to a better night’s sleep. As far as the snoring? Dr. Smith suggested trying a nightly regimen of nasal spray and allergy tablets, along with tilting up the head of my mattress a bit.
And if both these solutions work, she’ll have improved not only my sleep, but my husband’s.
Find out how other third-shift workers cope with being awake when everyone else is asleep.
The wellness you need, in a style you’ll love — delivered.
Sign up to have PA Health sent to your mailbox or inbox 4 times a year, for free.
